Contributor: Dr. Alison Baker

Contributor: Dr. Alison Baker

Recognizing, structuring, teaching, and integrating IPC explicitly into office workflow improves patient outcomes, learner development, and physician sustainability.
Practical Strategies for Preceptors

References & Further Reading
Contributor: Dr. Cindy Donaldson
Summary:
Embracing uncertainty boosts resilience, sharpens decision-making, and improves patient outcomes. Approaching patient encounters that are not clear cut (so many!) with a sense of curiosity and a willingness to look beyond initial impressions helps us manage vague descriptions and conflicting information. Managing uncertainty is a skill that improves with practice and reflection, enhancing what we do, making us better advocates for our patients.
Infographic:
This infographic highlights strategies for managing clinical uncertainty, including a useful mnemonic to help find certainty within uncertainty.

Contributor: Dr. Karthiha Raveenthiran
Asynchronous e-learning modules offer an efficient way to teach our learners important concepts, allow educators to reach more learners, and provide flexibility for learning.
Summary:
E-learning designers should develop clear goals relevant to their learners, engage in thoughtful selection of the learning platform, incorporate interactive modules and provide opportunities for learners to continue their learning beyond the module. This article explores 12 tips that can help medical educators use best practices to design, develop, implement, and continually improve e-learning modules.
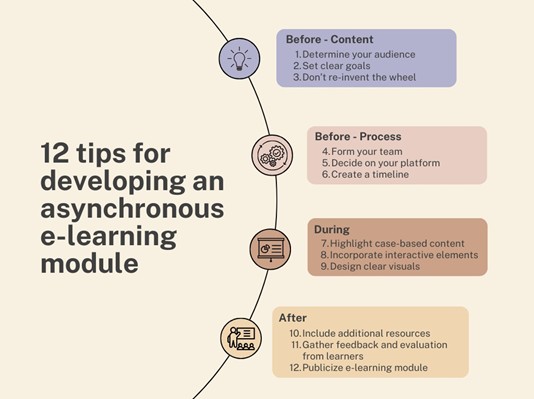
Link to Resource:
Paniszyn, L., Daddario, S., Colocci, I., Ibikunle, O., & Schwartz, A. W. (2026). Twelve tips for creating asynchronous e-learning modules in health professions education. Medical Teacher, 48(1), 25–30. https://doi.org/10.1080/0142159X.2025.2505120
Contributor: Dr. Nadine Abu-Ghazaleh
Why this matters
Disability is a common human experience. A 2021 Canadian Medical Association survey found that 22% of physicians report a disability or chronic health condition, most of which are non-apparent. Yet medical education continues to be shaped by a “selfless superhuman” ideal that assumes unlimited stamina, constant availability, and no need for accommodation. This narrative fuels internalized, cultural, and systemic ableism—and creates barriers for learners and faculty alike.
What is the “selfless superhuman”?
Medical culture continues to reflect an outdated “selfless superhuman” ideal that prioritizes endurance over wellbeing. We must challenge the stereotype that a “good doctor” is endlessly resilient, requires no rest, never gets sick, and consistently places personal needs last. By questioning how we define, model, and reward excellence, we can begin to recognize not only the systemic roots of this problem, but also the ways internalized ableism is perpetuated through our own clinical practices, teaching behaviours, and evaluative feedback.Creating space for this reflection is essential to fostering psychologically safe environments for learners, faculty, and all health-care allies.
What can you do?
Medical educators hold real power: in evaluation, scheduling, curriculum design, and culture-setting. Moving from reactive accommodationto proactive accessibility is a necessary step toward equity, wellness, and sustainable medical practice.
Practical Take-aways for Educators:
Key Take-away:
Accessibility is not about lowering standards—it’s about removing unnecessary barriers so people can meet them.
Key Definitions:
Resources:
References:
Canadian Medical Association. (2021). National physician health survey.
https://www.cma.ca/our-focus/physician-health-and-wellness/national-physician-health-survey Ontario Human Rights Commission. (n.d.). Policy on ableism and discrimination based on disability.
https://www.ohrc.on.ca/en/policy-ableism-and-discrimination-based-disability
Jain, N. R. (2022). The capability imperative: Theorizing ableism in medical education. Social Science & Medicine, 315, 115549.
https://doi.org/10.1016/j.socscimed.2022.115549
Centers for Disease Control and Prevention. (2023). Disability and health overview.
https://www.cdc.gov/ncbddd/disabilityandhealth/disability.html
Contributors: Courtney Manser, MD, CCFP (PC) and Alexis Milligan, M.IDST
Take Away Tidbits
The Five Modes of Communication
Take a moment to consider how you are communicating your words through the other modes. This includes how you are moving your body, the tone of your voice, and being aware of jumping to conclusions or assuming aspects in others that may not be the truth.
Try to balance being on receive as much as transmit and help activate listening in others.
Remember that breakdown of communication can often be something as simple as intention vs impact. Sometimes what we intend does not have the impact we want and vice versa.
How to Re-Centre Ourselves
Picture this: You’ve been on your feet all day, running from room to room. You’re behind. You’ve had at least one difficult patient encounter. You’re tired, both physically and emotionally. How do you continue to see patients without allowing your physical presence and non-verbal communication to affect how your patient perceives the interaction? What you are “giving off” is much more than the words you say. Take a deep breath and do the following:
The 5 points
If you can, take three deep breaths thinking of these five points and add a gentle secret smile.
Adaptability, Repetition, & Play
Playing is not always a reference to fun and games. It is a useful tool to help us adapt to something new, or work with rapid changes in a more positive way.
When you need to engage in seeing multiple patients, or feel like you are a broken record, ask yourself to find one thing that is different, unique, or special with each repetition.
Non-technical Skills
Bringing equal value to non-technical skills is an essential part of developing a whole-system approach to medical practice. They not only improve patient satisfaction and outcomes but also improve overall physician health and wellbeing.
Non-technical skills are easy to learn, and with practice they can become second nature
For more information on ‘Theatre of Medicine” through the Shaw Festival, please visit:
https://www.shawfest.com/theatre-of-medicine
References
Contributor: Amie Davis
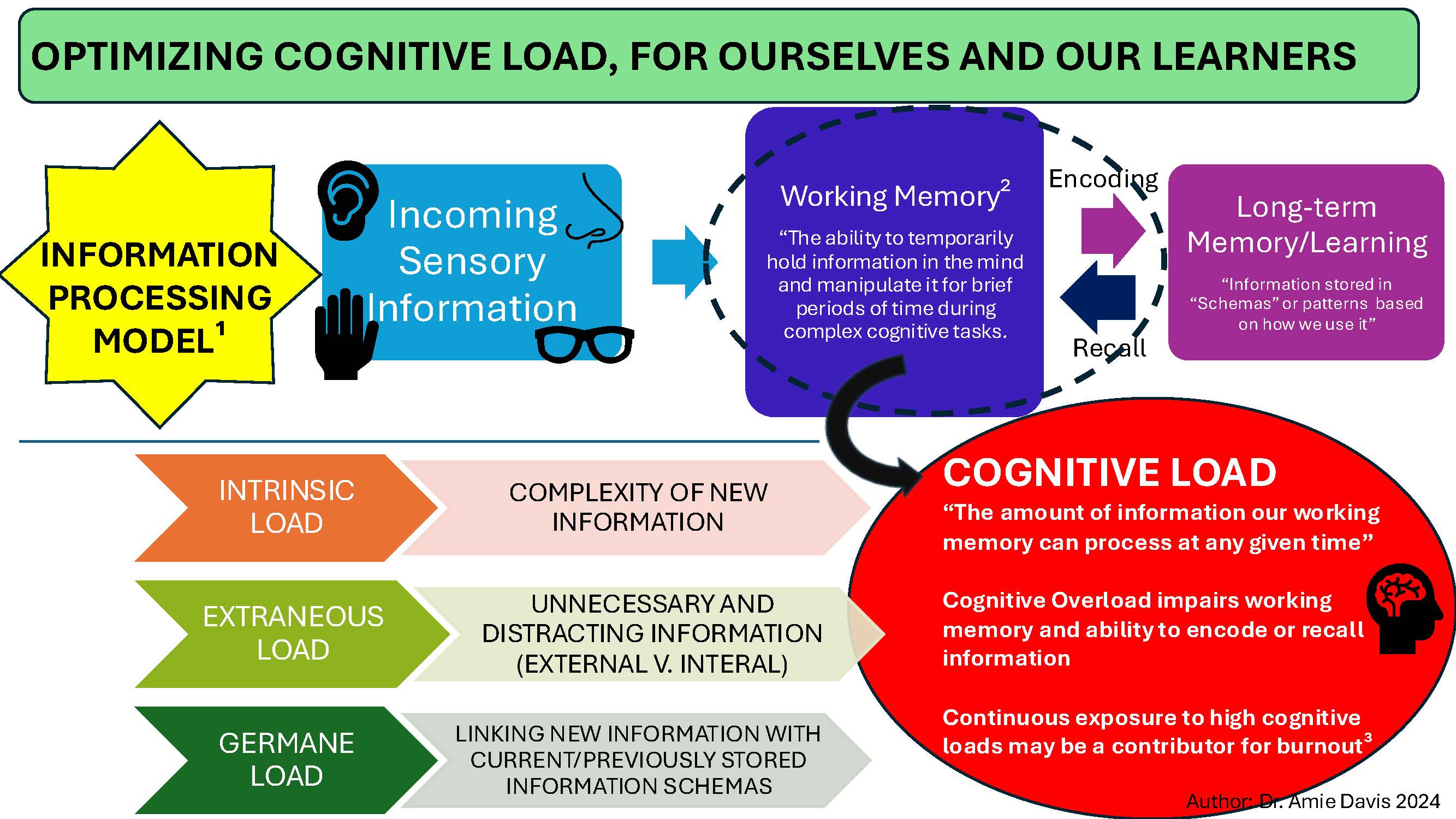
1- DECREASE INTRINSIC LOAD – “COMPLEXITY OF NEW INFORMATION”
• Use a spiral curriculum where learners are introduced and re-introduced to increasingly complex topics and encounters
• Encourage continuity with patients over time (allowing familiarization with complexity)
• ”Chunk” or “Sort” encounter into smaller pieces (e.g. Sort information by system)
2. DECREASE EXTRANEOUS LOAD – “UNNECESSARY AND DISTRACTING INFORMATION”
• EXTERNAL EXTRANEOUS LOADS
Optimize learning environment: Decrease interruptions (pages, message alerts, voice interruptions) during a tasks. Ensure all equipment is available and ready including technology and charting equipment. Clearly mark/hold times for tasks that can be seen and respected by others
• INTERNAL EXTRANEOUS LOADS
Manage fatigue – Micro-breaks between tasks to allow re-focus, allow time for nutrition and “bio-breaks”, ensure adequate time held in the day for the tasks needed (so that can be present and not focused on “what comes next/feeling rushed”), wear clothing that is comfortable and adjustable to temperature throughout the day
3. INCREASE GERMANE LOAD – “LINKING NEW INFORMATION WITH CURRENT/PREVIOUSLY STORED INFORMATION SCHEMAS”
• Introduce learning aids (e.g. Mnemonics, rhymes, common links, pattern recognition)
• Link to similar previous presentations or patients seen in the past (also increases spiral learning)
• Use low-fidelity simulation to high fidelity (patient encounters) when possible (e.g. Practice first)
References:
1. Atkinson,R.C and Shiffrin, R.M.(1968). Human memory: A proposed system and its control processes. The psychology of learning and motivation Vol.2 (89-195)
2. Baddeley, A.D. Working Memory. Phil. Trans.R.Soc.Lond.B. Vol 302,311-324(1983)
3. Steven E Roskos, Laurie Fitzpatrick, Bengt Arnetz, Judy Arnetz, Shiva Shrotriya, Elizabeth Hengstebeck, Complex patients’ effect on family physicians: high cognitive load and negative emotional impact, Family Practice, Volume 38, Issue 4, August 2021, Pages 454–459,https://doi.org/10.1093/fampra/cmaa137